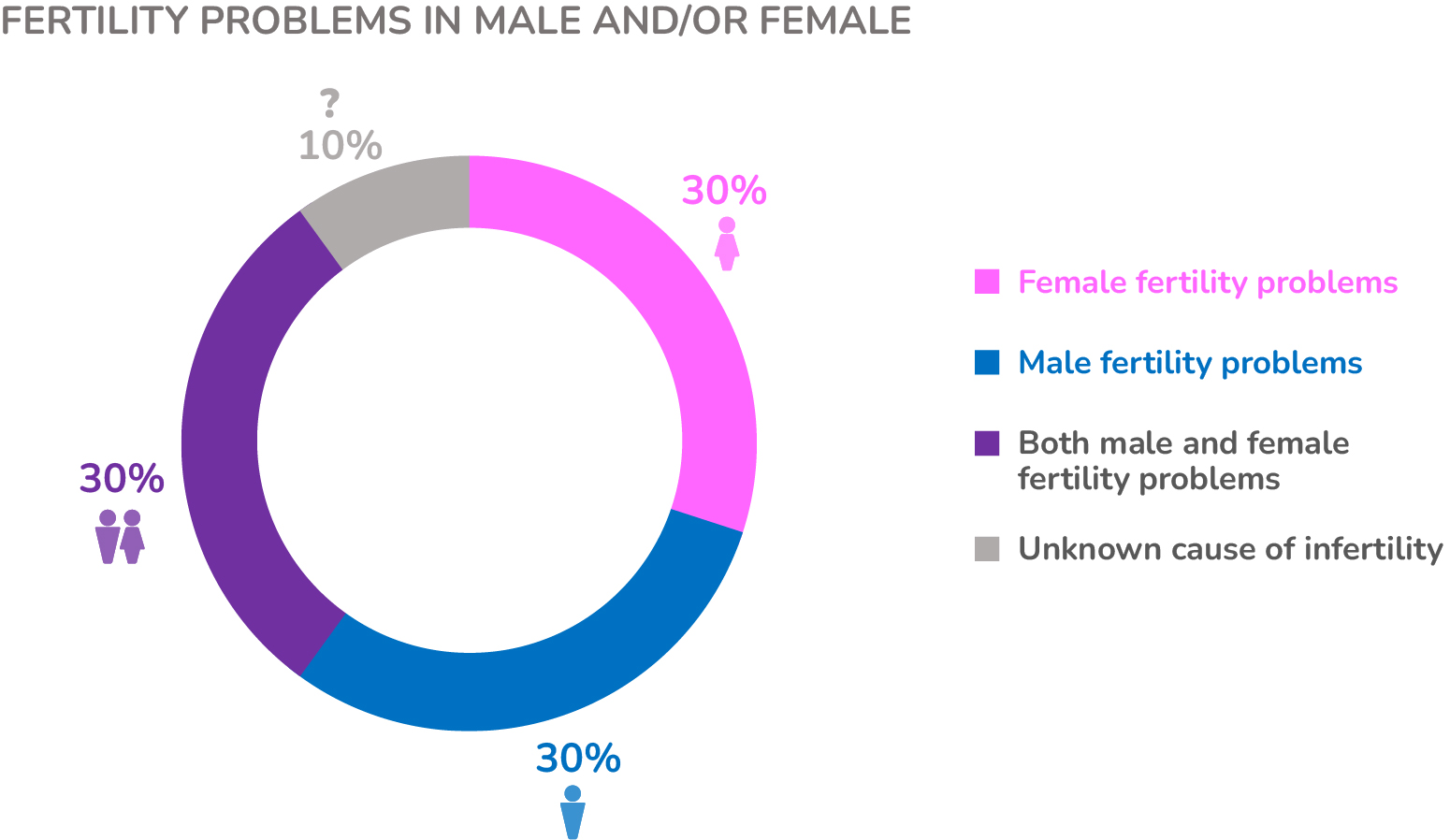
Polycystic Ovary Syndrome (PCOS) is one of the most common causes of infertility in woman of reproductive age. The percentage of woman with a PCOS ranges from 5% to 20%, depending on diagnostic criteria, and at least 70% of women with PCOS are not diagnosed by their primary care physician.
Although PCOS has been studied extensively for years, many aspects regarding causes, diagnosis, symptoms, complications and effective treatment remain unknown. There is evidence that a diverse set of genetic and environmental factors play an important role in the development of this syndrome. Furthermore, women with PCOS have a hormonal imbalance and other metabolic problems that could adversely affect their health. While PCOS is a frequent cause of infertility, the good news is that it can be treated with specific medications.
Symptoms of PCOS
Symptoms associated with PCOS typically first surface during adolescence and then worsen over time. Common problems include high testosterone levels, irregular menstrual cycles (infrequent periods, light or little bleeding, or a heavy flow), chronic anovulation, and frequently infertility.
During adolescence, the most common clinical sign of high testosterone level is male-pattern facial hair. Sometimes this symptom might be associated with other symptoms, such as moderate-severe acne and a receding hairline. Importantly, obesity is a significant risk factor associated with PCOS and also implicated in infertility in general.
Diagnosis and therapy
A medical evaluation should be the first course of action for any woman showing signs/symptoms of PCOS. This will usually include a physical exam, discussion of family history and laboratory tests.
Ovarian and pelvic ultrasonography may also be used to assess each ovary’s volume and antral follicle count. In addition, hormonal testing is usually required to determine the extent of ovarian problems.
Nonetheless, it can be challenging to diagnose PCOS in young girls (especially in the two years after they get their first period), since PCOS symptoms may resemble normal puberty. The medical evaluation combined with lab results can assist a physician in determining the extent of the PCOS as well as the best treatment strategy.
There is no one right way to treat PCOS. Instead, medications must be tailored to each woman’s preferences, risk profile, and treatment goals. Medications that are sometimes used to treat PCOS include Metformin, a diabetes medication, and combined oral contraceptive pills. Other frequently prescribed therapies include spironolactone as well as topical treatments for excessive facial hair and acne. For women who are planning to conceive, oral ovulatory agents (clomiphene citrate or letrozole) are often used as well.
PCOS and infertility
Since it is frequently associated with anovulation and ovulatory dysfunction, PCOS is the most common cause of infertility among women. Women suffering from PCOS may also be at risk of increased complications during pregnancy. For these reasons, women trying to conceive should consider treatment with an oral ovulatory agent, such as clomiphene citrate or letrozole. Approximately 50% of ovulating patients on clomiphene will conceive after three to five treatment cycles. If the patient fails to either ovulate or conceive after six months of clomiphene or letrozole, other solutions can be considered, such as gonadotropin ovulation induction or laparoscopic ovarian drilling. Additionally, women who do not get pregnant with ovulation induction can choose to proceed to in vitro fertilization and embryo transfer.
Comorbidities
In some patients, PCOS could be associated with metabolic and cardiovascular disorders and with psychological issues that adversely affect a women’s quality of life. Possible PCOS complications include insulin resistance, hyperinsulinemia, obesity, increased risk of type 2 diabetes mellitus, metabolic syndrome, hypertension, cerebrovascular accidents, cardiovascular disease and deep vein thrombosis. Moreover, depression and anxiety are common in PCOS patients. Finally, subjects affected by PCOS may be at increased risk of endometrial and ovarian – but not breast – cancer.
Preventive measures
Since being overweight is considered a risk factor for PCOS, lifestyle interventions are considered essential for the prevention of this syndrome. Strategies to improve lifestyle include a healthy diet (also fertility diet) and physical exercise. Moreover, behavioural interventions might be helpful in managing psychological factors – anxiety, depression, body image concerns and disordered eating – which can negatively impact the quality of life. A good lifestyle is also important for improving fertility.
In conclusion, the early diagnosis of Polycystic Ovary Syndrome and the initiation of specific treatment are essential steps not only for women trying to conceive, but also for all patients with PCOS as it could adversely affect physical and mental health.
References
- Teede HJ, Misso ML, Costello MF, et al; International PCOS Network. Recommendations from the international evidence-based guideline for the assessment and management of polycystic ovary syndrome. Fertil Steril. 2018;110(3):364-79.
- Vander Borght M, Wyns C. Fertility and infertility: Definition and epidemiology. Clin Biochem. 2018; 62:2-10.
- Deswal R, Narwal V, Dang A, Pundir CS. The Prevalence of Polycystic Ovary Syndrome: a brief systematic review. J Hum Reprod Sci. 2020;13(4):261-71.
- Azziz R, Carmina E, Chen Z, et al. Polycystic ovary syndrome. Nat Rev Dis Primers. 2016; 2:16057.
- Witchel SF, Oberfield SE, Peña AS. Polycystic Ovary Syndrome: pathophysiology, presentation, and treatment with emphasis on adolescent girls. J Endocr Soc. 2019;3(8):1545-73.
- Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group. Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome. Fertil Steril. 2004;81(1):19-25.
- Infertility Workup for the Women’s Health Specialist: ACOG Committee Opinion, Number 781. Obstet Gynecol. 2019;133(6): e377-84.
- McDonnell R, Hart RJ. Pregnancy-related outcomes for women with polycystic ovary syndrome. Womens Health (Lond). 2017;13(3):89-97.
- Tomlinson JA, Pinkney JH, Evans P, et al. Screening for diabetes and cardiometabolic disease in women with polycystic ovary syndrome. The British Journal of Diabetes & Vascular Disease, 2013; 13(3), 115-23.
- Kshetrimayum C, Sharma A, Mishra VV, Kumar S. Polycystic ovarian syndrome: Environmental/occupational, lifestyle factors; an overview. J Turk Ger Gynecol Assoc. 2019;20(4):255-63.
- Ramezani Tehrani F, Amiri M. Polycystic Ovary Syndrome in Adolescents: Challenges in Diagnosis and Treatment. Int J Endocrinol Metab. 2019;17(3):e91554.
- Infertility Workup for the Women’s Health Specialist: ACOG Committee Opinion, Number 781. Obstet Gynecol. 2019;133(6):e377-84.
- Çelik Ö, Köse MF. An overview of polycystic ovary syndrome in aging women. J Turk Ger Gynecol Assoc. 2021;22(4):326-33.
- Al Khalifah RA, Florez ID, Zoratti MJ, Dennis B, Thabane L, Bassilious E. Efficacy of Treatments for Polycystic Ovarian Syndrome Management in Adolescents. J Endocr Soc. 2020;5(1): bvaa155.
- Aversa A, La Vignera S, Rago R, et al. Fundamental concepts and novel aspects of Polycystic Ovarian Syndrome: Expert Consensus Resolutions. Front Endocrinol (Lausanne). 2020; 11:516.